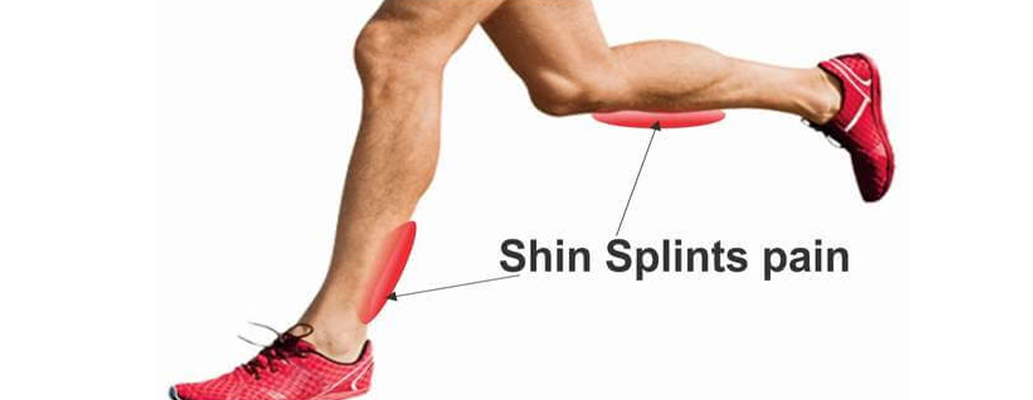
Overview
Usually referred to as medial tibial stress syndrome, shin splints are a medical condition that afflicts sports, dancers, and runners most of the time. Usually, the phrase for this condition is shin splints.
Usually, from excessive use, this ailment causes pain along the inner edge of the shinbone. Knowing the specifics of shin splints will enable you to control and avoid this uncomfortable disorder, thereby enabling your continued activity and health.
Symptoms
One of the most noticeable symptoms of shin splints is a painful sensation running down the inner part of the affected leg. In most cases, this discomfort is worse while you perform physical activity, although it could get better when you relax. Additional symptoms might be minor swelling, pain, and weakness in the region of injury. In order to provide quick and successful treatment, it is essential to identify these symptoms at an earlier phase.

Causes
Shin splints may develop from excessive stress imposed on the shinbone and the connective tissues binding muscles to the bone. Some common reasons are:
l Overtraining:
Putting yourself to an excessive degree or for an extended time.
l Flat
Feet or High Arches: Wearing worn-out shoes or ones without enough
support might lead to foot issues.
l High
arches or flat feet: The lower limbs can be stressed more by
confident foot kinds.
l Running
on Hard Surfaces: Concrete and other similar surfaces can
increase the risk of shin injury.
Developing a better understanding of these factors can assist in implementing techniques to reduce the likelihood of shin splints.

Risk Factor
Shin splints are more likely to occur if you have certain risk factors, such as:
l High-impact
sports: Running, soccer, and basketball.
l Poor
Running Mechanics: inappropriate posture or gait.
l Previous
Injuries: A history of lower leg problems, including shin
splints or other injuries.
l Inadequate
Warm-Up: Ignoring appropriate warm-up routines
before intense physical activities.
Physical therapy for Shin splints
Consultation with a physio for shin splints can be of great assistance in the management and prevention of this condition. With the help of a treatment program developed by a physiotherapist, which includes customized massages and exercises, one can address both the shin muscles and biomechanics.
What are Symptoms of shin splints?
People with shin splints will experience some of the following symptoms:
- a dull ache in the front part of the lower leg
- pain that develops during exercise
- pain on either side of the shin bone
- muscle pain
- pain along the inner part of the lower leg
- tenderness or soreness along the inner part of the lower leg
- swelling in the lower leg (usually mild if present)
- numbness and weakness in the feet
- severe pain in your shin after a fall or accident
- a shin that feels hot
- a shin that is visibly swollen
- pain in your shins even when you are resting.
How are shin splints diagnosed?
Shin splints is diagnosed via physical examination and evaluation of your medical history. The physiotherapists will take notes about your training schedule, workplace activities, and may also want to know whether you have recently begun a new exercise regime that requires running or jumping.
The physical examination allows us to see exactly where your leg hurts. We may move your ankle in different positions and have you hold your foot against applied pressure. By stretching the tibialis muscles, and by feeling where these muscles attach on the tibia, we can begin to tell where the problem is.
What are the symptoms of plantar fasciitis?
Common symptoms include mild pain on the bottom of the heel, especially when taking your first steps of the day. Often, symptoms improve only to worsen later in the day. This happens due to over-stressing of the plantar fascia causing a chronic healing response at the attachment to the bone that may remain sore for months.
How is Shin splint treated?
Like many degenerative conditions, it is caused by wear and tear of the fibers of the fascia. One of the most common causes, is a strain to the tissue due to a specific activity combined with improper or inadequate flexibility of the Achilles tendon and the calf muscle. Other causes include a pinched nerve in the heel region, thinning of the heel fat pad, or a stress fracture of the heel bone.
When should you see the physiotherapist?
Reducing Inflammation
The treatment focuses on reduction of inflammation and pain relief. Patients suffering from shin splints receive Ultrasound treatments, effective in halting pain and inflammation. To speed your recovery the physiotherapists may also use deep tissue release technique along the junction where the sore tibialis muscle meets the tibia, followed by gentle stretching of the calf and tibialis muscles.
Foot Support
We will evaluate your posture and alignment to see if you have problems with pronation (arch flattening), a condition that we commonly see associated with posterior shin splints. Sometimes a small heel wedge, placed under the inside edge of the heel, is enough to ease tension on the posterior tibialis muscle. For more severe problems of pronation, we may recommend foot orthotics to support the arch and reduce stresses on the posterior tibialis muscle.
How long is the shin splint treatment?
The length of the physiotherapy program varies for each patient depending on unique and individual characteristics of the condition but as a guideline you might expect four to six weeks to your recovery and rehabilitation.
How can shin splints can prevented?
- Analyze your movement. A formal video analysis of your running technique can help to identify movement patterns that can contribute to shin splints. In many cases, a slight change in your running can help decrease your risk.
- Avoid overdoing. Too much running or other high-impact activity performed for too long at too high an intensity can overload the shins.
- Choose the right shoes. If you're a runner, replace your shoes about every 350 to 500 miles (560 to 800 kilometers).
- Consider arch supports. Arch supports can help prevent the pain of shin splints, especially if you have flat arches.
- Consider shock-absorbing insoles. They might reduce shin splint symptoms and prevent recurrence.
- Lessen the impact. Cross-train with a sport that places less impact on your shins, such as swimming, walking or biking. Remember to start new activities slowly. Increase time and intensity gradually.
- Add strength training to your workout. Exercises to strengthen and stabilize your legs, ankles, hips and core can help prepare your legs to deal with high-impact sports.